Chronic pain relief involves a comprehensive approach using medical treatments, holistic therapies, and lifestyle changes to reduce persistent pain lasting three months or longer. Here are the most effective options:
Medical Treatments:
- NSAIDs and acetaminophen for mild-moderate pain
- Antidepressants and anti-seizure medications for nerve pain
- Interventional procedures like nerve blocks and injections
- Opioids as last resort for severe cases
Non-Medical Approaches:
- Physical therapy and gentle exercise
- Mind-body techniques like mindfulness and CBT
- Advanced technologies like scrambler therapy (80-90% success rate)
- Acupuncture, massage, yoga, and tai chi
Living with chronic pain affects 50 million Americans, making it one of the most common health challenges we face today. Unlike acute pain that signals injury and heals within weeks, chronic pain persists for months or years – often long after the original cause has resolved.
This persistent pain creates a vicious cycle. Chronic pain can limit quality of life and lead to complications beyond physical symptoms. As research shows, people with chronic pain frequently experience depression, anxiety, and sleep problems that can actually make the pain worse.
The impact goes far beyond physical discomfort. Chronic pain affects your ability to work, maintain relationships, and enjoy activities you once loved. It can leave you feeling isolated and hopeless, wondering if relief will ever come.
But here’s what’s important to understand: effective chronic pain management is possible. Today’s treatment approaches recognize that chronic pain isn’t just about damaged tissue – it’s about how your nervous system processes and amplifies pain signals. This understanding has opened doors to new treatments that address both the physical and emotional aspects of persistent pain.
Whether your pain stems from arthritis, fibromyalgia, nerve damage, or has no clear cause, there are proven strategies that can help you reclaim your life. The key is finding the right combination of treatments that work for your unique situation.
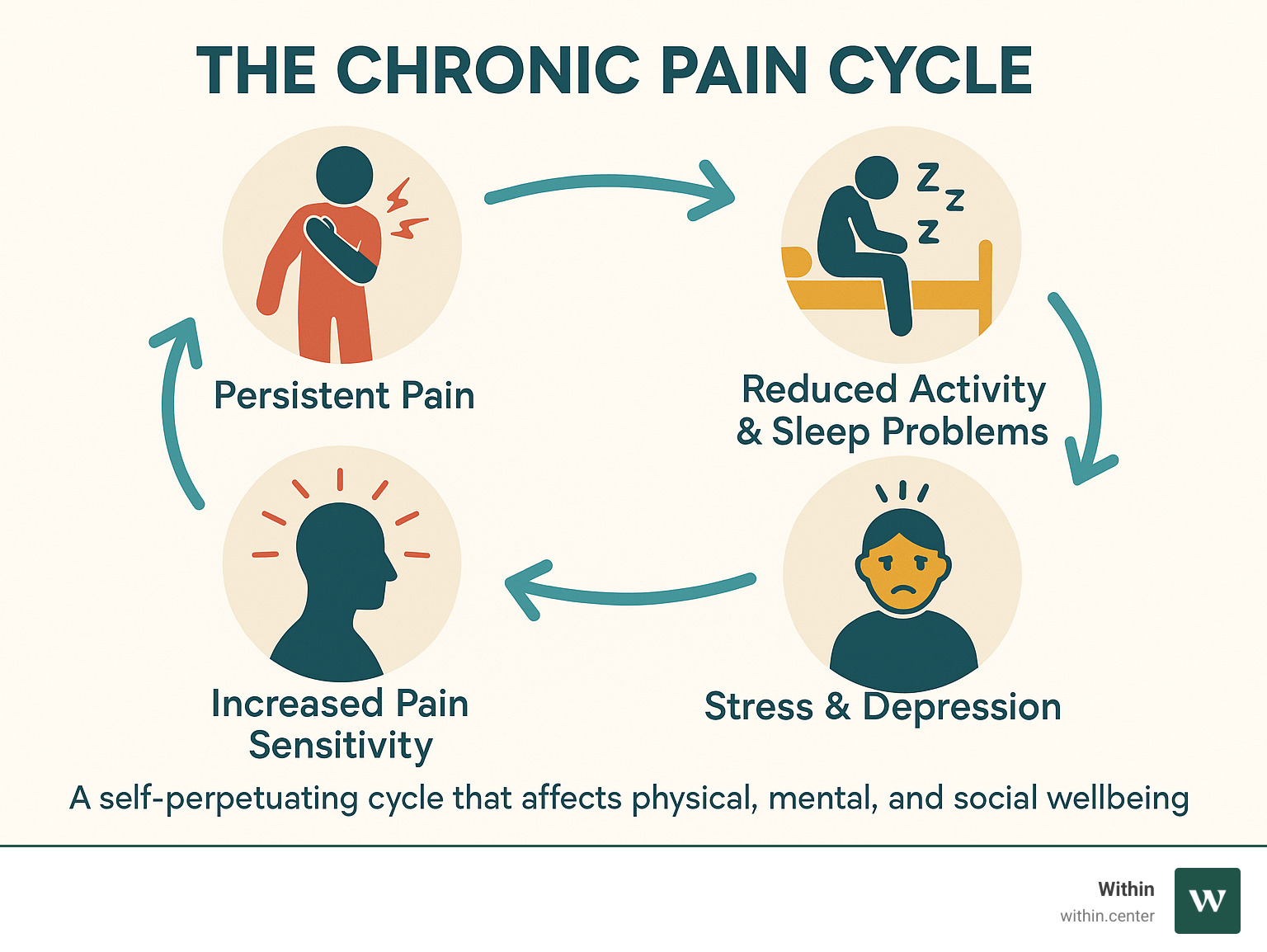
Understanding Chronic Pain: The What, Why, and How It Affects You
When you’re living with chronic pain, it can feel like your body has betrayed you. But understanding what’s actually happening can be the first step toward finding relief. Let’s explore the science behind persistent pain and how it might be affecting your daily life.
What is Chronic Pain and Its Causes?
Think of your nervous system as your body’s alarm system. When you touch something hot or twist your ankle, pain signals race through your nervous system to warn you of danger. This is acute pain – sharp, immediate, and usually temporary.
Chronic pain is different. It’s pain that lasts 3+ months or longer, often continuing long after the original injury has healed. Sometimes it develops from an injury or infection that never quite resolved. Other times it stems from ongoing conditions like arthritis, fibromyalgia, or nerve damage. And frustratingly, chronic pain sometimes has no clear cause at all.
Here’s what makes chronic pain so complex: your body’s alarm system gets stuck in the “on” position. Even when there’s no immediate danger, the pain signals keep firing. This happens through a process called central sensitization, where your brain and nervous system become hypersensitive to pain. It’s like having a smoke detector that goes off every time you make toast – the system meant to protect you becomes overactive.
The scientific research on chronic pain continues to reveal new insights about how these persistent pain signals develop and why they’re so challenging to treat.
Common Risk Factors and Triggers
While chronic pain can strike anyone, certain factors make some people more vulnerable. Age plays a role – about 65% of Americans over 65 report chronic pain as wear and tear accumulates over time.
Gender differences are also significant. Women experience chronic pain more frequently than men and face higher risks for conditions like fibromyalgia and migraines. Genetics can predispose you to certain pain conditions, while previous injuries may leave lasting changes in how your nervous system processes pain.
Perhaps most importantly, psychological factors like stress and depression don’t just accompany chronic pain – they can actually make it worse. Your mind and body are deeply connected, and emotional distress can amplify physical pain signals. It’s not “all in your head,” but your mental state genuinely affects how your brain processes pain.
The Widespread Impact on Daily Life
Living with chronic pain touches every corner of your life. The physical limitations are often the most obvious – simple tasks like grocery shopping or playing with your children can become overwhelming challenges. But the ripple effects go much deeper.
The emotional toll can be devastating. Research shows that 25% of chronic pain patients develop depression, while two-thirds struggle with concentration and memory problems. When pain never gives you a break, it’s natural to feel frustrated, anxious, or hopeless.
Social isolation often follows. You might start declining invitations or avoiding activities you once enjoyed. Friends and family may not understand why you look fine but feel terrible, leading to strained relationships and loneliness.
Work challenges are common too. About 25% of people with chronic pain have to leave their jobs, while 50% of those still working report they can’t perform at their best. The financial stress only adds to the burden.
Perhaps most concerning is the link between chronic pain and mental health conditions, including PTSD. The constant stress of living with pain can trigger or worsen psychological symptoms, creating a cycle where pain and mental health issues feed off each other.
Understanding these connections is crucial for effective chronic pain relief. When you recognize that chronic pain affects your whole person – not just the part that hurts – you can begin to see why comprehensive treatment approaches often work best. Resources like Coping with Chronic Pain can provide additional support as you steer these challenges.
The good news? Recognizing these patterns is the first step toward breaking them. Once you understand what you’re dealing with, you can start building a plan to reclaim your life from chronic pain.
A Spectrum of Solutions: Medical and Pharmacological Treatments
When it comes to chronic pain relief, there’s no “one-size-fits-all” solution. It’s truly a journey to find what works best for you. Many people find that a thoughtful combination of approaches yields the best results, custom to your unique needs and the kind of pain you’re experiencing. Medications can play a significant role for many, but it is important to understand their benefits, potential risks, and how they fit into a broader plan that includes movement, mind-body work, and lifestyle changes.
Over-the-Counter and Prescription Medications
These are often the first steps many people take to manage pain. They range from options you can pick up at the pharmacy to stronger medications that require a prescription. Here are common options and how they compare:
| Medication Type | How It Works | Benefits | Risks and Cautions | Best Use Cases |
| NSAIDs (e.g., ibuprofen, naproxen; some prescription-strength) | Reduce inflammation by inhibiting COX enzymes | Helpful for inflammatory pain (arthritis, strains, menstrual pain); reduce swelling | Stomach irritation/bleeding, kidney strain, increased blood pressure, possible heart risks; avoid or use cautiously with GI, kidney, or heart disease | Short courses for flares of inflammatory pain; use the lowest effective dose |
| Acetaminophen (paracetamol) | Acts centrally to reduce pain and fever (not anti-inflammatory) | Gentle on the stomach; useful when inflammation is not the main driver | Liver toxicity at high doses or with alcohol; keep total daily dose within recommended limits and consider all combination products | Mild to moderate pain (headache, osteoarthritis) when NSAIDs are not appropriate |
| COX-2 inhibitors (e.g., celecoxib) | Target COX-2 to lower inflammation with less GI irritation | Lower risk of stomach ulcers vs. traditional NSAIDs | Potential cardiovascular risks; use under medical guidance, especially with heart disease risk | Chronic inflammatory conditions when NSAIDs help but GI side effects are a concern |
As with all medications, dosing and duration should be individualized. Discuss your medical history and other medicines or supplements you take with your clinician to avoid interactions.
Antidepressants and Anti-Seizure Medications for Nerve Pain
Neuropathic pain (from conditions like diabetic neuropathy, shingles/postherpetic neuralgia, spinal nerve compression, or fibromyalgia) often responds poorly to standard painkillers. Certain antidepressants and anti-seizure medications can help by modulating how the nervous system processes pain signals.
- Antidepressants: Tricyclics (e.g., amitriptyline, nortriptyline) and SNRIs (e.g., duloxetine, venlafaxine) can reduce nerve pain and improve sleep and mood, which further supports pain relief. See an overview at Antidepressants for chronic pain.
- Anti-seizure medications: Gabapentin and pregabalin can calm overactive nerve signaling and reduce burning or electric-shock sensations common in neuropathic pain.
These medicines often start at low doses and are slowly increased to balance benefit and side effects (like drowsiness, dry mouth, or dizziness). Because pain is intertwined with mood and stress, pairing medication with psychotherapy, mindfulness, and integration support can improve outcomes. For perspective on the value of therapy within a broader healing plan, see More info about the importance of therapy.
The Role and Risks of Opioids
Opioids can provide powerful relief for severe, acute pain and for carefully selected cases of chronic pain when other treatments fall short. However, for chronic non-cancer pain, opioids carry significant risks: tolerance, dependence, constipation, hormonal changes, heightened pain sensitivity over time, and addiction and overdose risk.
If opioids are considered, they should be used at the lowest effective dose, with clear functional goals, time-limited trials, and close monitoring. They are generally a last-resort option after safer treatments are tried or used in combination with non-opioid strategies. For context on comprehensive pain strategies, see More info on moving beyond opioids.
Interventional Procedures
When medication and conservative therapies are not enough, image-guided procedures can target pain at its source:
- Epidural steroid injections: Reduce inflammation around irritated spinal nerves (e.g., sciatica).
- Facet or sacroiliac joint injections: Diagnose and treat pain arising from spinal or pelvic joints.
- Nerve blocks: Temporarily interrupt pain signaling to help both diagnosis and relief.
- Radiofrequency ablation (RFA): Uses heat to disrupt pain-transmitting nerve fibers for longer-lasting relief (often 6–12 months) in select joint or spine pain.
- Pain pumps (intrathecal therapy): Deliver tiny doses of medication directly to the spinal fluid for severe, refractory pain under specialist care.
These procedures are performed by trained clinicians (often anesthesiology, pain medicine, or physical medicine and rehabilitation specialists). Benefits can include reduced pain and improved function, sometimes enabling lower doses of oral medications. As with any procedure, discuss risks, expected duration of benefit, and how each fits into your overall plan.
Putting it together: Medications and procedures are most effective when paired with physical therapy, sleep and stress skills, and meaning-making work that calms the nervous system and supports change. A team-based approach helps you weigh the tradeoffs of each option and adjust the plan as your body and life evolve.



